The kidneys have so many jobs, more than just creating urine and ridding the body of toxins. They also manage hydration, blood pressure, red blood cell production, pH balance in the blood, calcium, and phosphorus balance, and more. So, when they don’t work so well, there are many body systems which can be affected.
The filtration unit in a kidney is called the nephron. Over time, these start to die off because of the normal wear and tear of living. Animals and humans are usually born with 2 kidneys packed full of nephrons, and we actually only need the equivalent of 1/3 of one kidney’s worth for our kidneys to work normally. However, there may come a time when your pet just doesn’t have enough working nephrons to sustain normal kidney function. In the early stages this is called Renal Insufficiency (renal means kidney) and means your pet’s kidneys need help to do their job. Chronic Renal Disease means that your pet has had kidney disease for some time.
What do the kidneys actually do?
Conserving Water
The kidneys concentrate urine, so the body gets to keep most of the water that is ingested. The smallest amount of water possible is used to help rid the body of unwanted toxins. Similarly, if your pet drinks too much water, they will produce more urine so that the bloodstream isn’t diluted too much. If the kidneys aren’t working too well, they can’t concentrate the urine. Your pet will produce more urine than normal and will therefore drink more water to balance this out.
Vet Test: Urine Specific Gravity (USG)
We will collect a sample of urine and measure how concentrated it is. Just as a comparison, water has a specific gravity of 1.000. Well concentrated urine has a USG of over 1.035. Dilute urine has a USG of less than 1.020.
Removing Toxins from the Body
When there isn’t enough blood flowing through the kidneys or if there aren’t enough nephrons doing their job, toxic waste starts to build up in the bloodstream. This is called azotaemia. When the toxin level gets too high, your pet will start to feel sick. This is called uraemia. Our job is to prevent the azotaemia getting to uraemic levels for as long as we can.
Vet test: Blood testing (Biochemistry)
We will collect a sample of your pet’s blood and run it through some machines in our in-house laboratory. We will be looking at a few markers to help us check for azotaemia and stage the kidney disease.
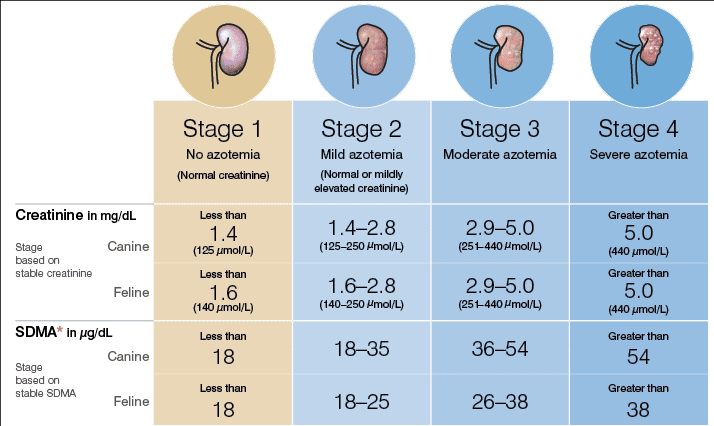
SDMA becomes abnormal much earlier than creatinine does and is a sign of early kidney disease when it is elevated.
BUN (blood urea nitrogen) is also elevated when the kidneys are not functioning well. It isn’t specific to kidney disease as it is also high just after eating a meal containing protein.
We will then use these results to determine how severe the kidney disease is.
Calcium/Phosphorus Balance
Too much or not enough of one or the other of these can cause crystals to start forming in tissues of the body. We will monitor the phosphorus level and will often use diet or medications to keep it in a reasonable range.
Sodium/Potassium Balance
The kidneys usually conserve potassium, so when they don’t function well the potassium levels start to drop, resulting in muscle weakness.
Blood Pressure Regulation
There are blood pressure receptors in the kidneys, so when the kidneys are damaged they will get damaged as well. The blood pressure can start to increase, which can damage the kidneys even more. We will sometimes want to measure your pet’s blood pressure if they are in the advanced stages of kidney disease.
Conserving Protein
When a part of the nephron called the glomerulus gets damaged, important proteins can leak from the bloodstream into the urine, and the body then cannot use these proteins for normal metabolic functions.
Vet test: Urine Protein:Creatinine Ratio (UPC)
We will sometimes send urine to the laboratory for a special test called Urine Protein:Creatinine ratio to determine how much protein is being lost in the urine.
Making Red Blood Cells
The kidneys make a hormone that tells the bone marrow to make more red blood cells when the levels get low. If the kidneys aren’t functioning properly this message doesn’t get through and your pet will develop a non-regenerative anaemia (this is a low red blood cell level that the body can’t fix).
Vet test: Blood Sampling (Complete Blood Count)
A Complete Blood Count (CBC) will tell us the levels of red and white blood cells, amongst other things. A Packed Cell Volume (PCV) is part of the CBC and is the measure of how many red blood cells are in your pet’s bloodstream.
Symptoms of Chronic Renal Disease
- Drinking more water than normal
- Urinating more often/having accidents
- Weight loss
- Not eating as much
- Vomiting
- Weakness
- Severely bad breath/mouth ulcers
Your pet may have only one or two of the above symptoms, but they will worsen as the kidney disease progresses. We may see none of the physical symptoms but diagnose early renal insufficiency on a routine wellness check. The earlier we diagnose renal disease, the more chance we have in slowing its progression.
Prevention and Treatment of Kidney Disease
Treatment in the early stages involves trying to prevent progression of kidney disease. Treatment in the later stages is about maintaining a quality of life for your pet.
Prevention in the early stages is all about weaning your pet on to a prescription diet designed specifically to decrease the pressure on the kidneys, and encouraging water intake. The diet will have controlled amounts of protein, and reduced levels of phosphorus and sodium, as well as important amino acids and essential fatty acids to help the body function well. Hills and Royal Canin both have prescription diets available. There are both biscuit (dry) and canned (wet) forms of food, with a range of flavours.
We recommend slowly weaning your pet onto the food as we don’t want them to develop an aversion to it. Mix with the existing food and change the ratio over 1-2 weeks.
We may not diagnose your pet with kidney disease until they are at stage 3 or 4, in which case they are often nauseous, anorexic, dehydrated and weak. They will need intense care in hospital which involves intravenous fluid therapy, antinausea medication, vitamin injections, pain relief and syringe feeding. We can often make a difference to their quality of life by doing this, but once they are discharged from hospital they will need ongoing care and careful monitoring as there is a high chance of relapse. The ongoing care may involve us teaching you how to administer subcutaneous fluids at home, regular visits for vitamin injections, constant dietary control and regular blood and urine tests. If your pet has other old-age disease processes such as arthritis we won’t be able to use the routine anti-inflammatory medication for this as it can affect the kidneys, so we will have to look at other options for this as well.
